Starting TRT without a fertility plan is one of the most expensive mistakes men make -- not in dollars, but in options. Exogenous testosterone shuts down the hormonal signals that drive sperm production, and for roughly 40% of men, the result is zero viable sperm within months.
The good news: this is a solved problem. Multiple proven strategies exist to preserve fertility while on TRT, recover sperm production after suppression, or protect your options before you ever start treatment. The key is making these decisions before they become emergencies.
This guide covers every fertility preservation strategy available to men on TRT -- from the biology of why suppression happens to the specific protocols clinicians use to prevent it.
Key Takeaways
- TRT suppresses sperm production in ~90% of men, with ~40% reaching complete azoospermia within 3-6 months
- HCG (500 IU, 2-3x weekly) concurrent with TRT is the frontline fertility preservation strategy
- Enclomiphene is an alternative that raises testosterone while preserving natural sperm production
- FSH combined with HCG recovers spermatogenesis in ~74% of men after testosterone-induced suppression
- Sperm banking before TRT is the only guaranteed insurance policy
- Recovery after stopping TRT takes 6-24 months, with 67-90% of men eventually recovering
How TRT Suppresses Fertility: The HPG Axis
Your reproductive system runs on a feedback loop called the hypothalamic-pituitary-gonadal (HPG) axis. Understanding this loop is essential to understanding why TRT suppresses fertility and how every preservation strategy works.
Here's the chain of command:
- Hypothalamus releases gonadotropin-releasing hormone (GnRH) in pulses
- Pituitary gland responds by secreting luteinizing hormone (LH) and follicle-stimulating hormone (FSH)
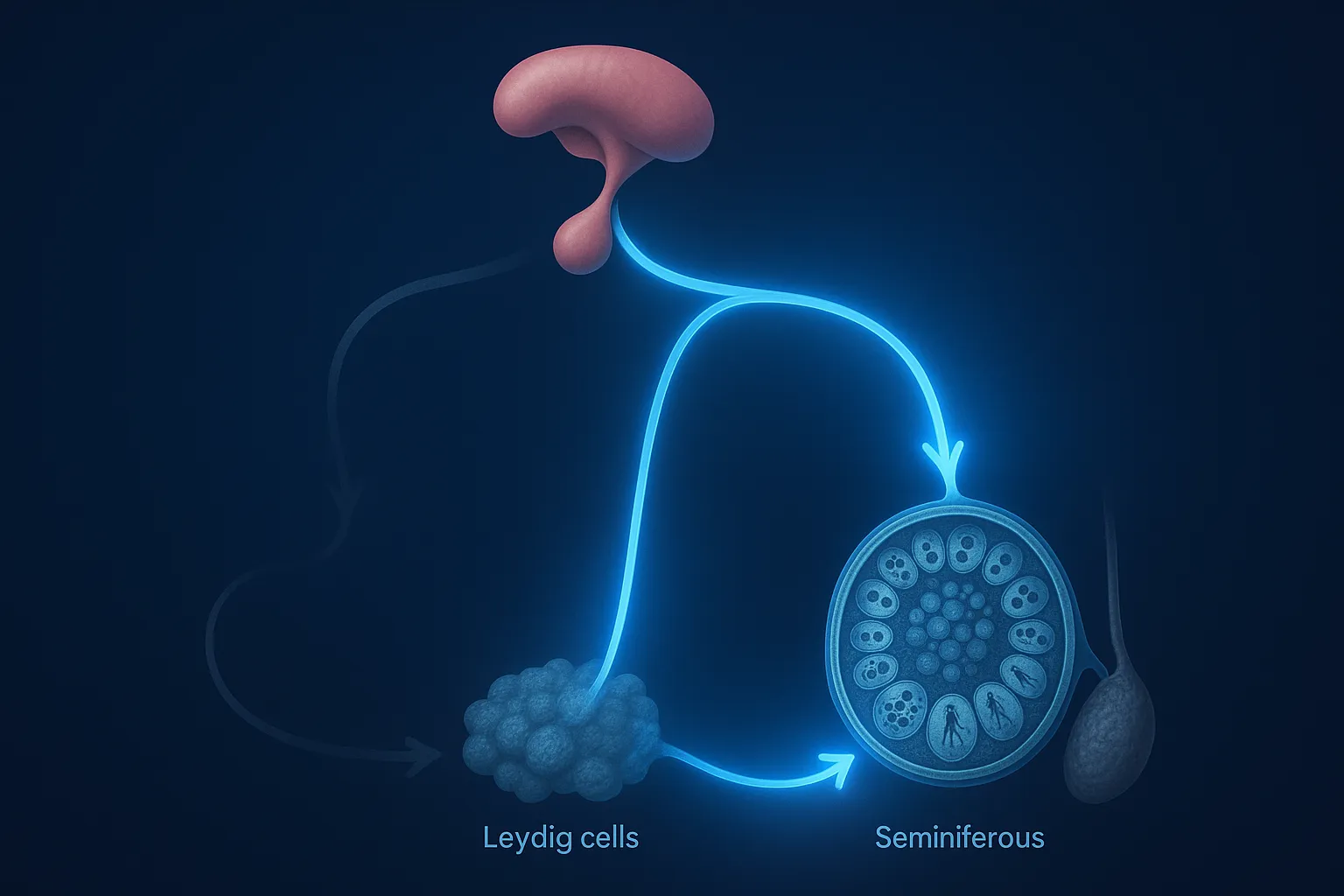
- LH tells Leydig cells in the testes to produce testosterone
- FSH drives Sertoli cells to support spermatogenesis (sperm production)
- Rising testosterone and estradiol signal the hypothalamus to slow GnRH release -- completing the feedback loop
When you inject exogenous testosterone, your blood levels rise well above what the hypothalamus expects. It detects the surplus and slams the brakes -- GnRH output drops to near zero. Without GnRH, the pituitary stops producing LH and FSH. Without LH and FSH, your testes lose both signals: the signal to produce testosterone internally and the signal to produce sperm.
The critical detail most men miss: spermatogenesis requires intratesticular testosterone (ITT) concentrations 50-100x higher than what circulates in the bloodstream. On TRT, ITT drops by 90-95% because the Leydig cells are no longer being stimulated. Even though your blood testosterone is high, your testicular testosterone collapses -- and that's what sperm production depends on [1].
This isn't a side effect or a complication. It's the predictable pharmacology of exogenous testosterone.
Timeline: How Fast Does Sperm Production Decline?
The suppression isn't instant, but it's faster than most men expect:
| Timeframe | What's Happening |
|---|---|
| Weeks 1-4 | LH and FSH begin declining. Intratesticular testosterone drops. No visible change in semen analysis yet. |
| Months 1-3 | Sperm concentration starts falling. Some men already show oligospermia (<15 million/mL). Testicular volume begins decreasing. |
| Months 3-6 | Most men reach severely oligospermic or azoospermic levels. About 40% have zero sperm on semen analysis. |
| Months 6-12 | Suppression deepens in late responders. Testicular volume may decrease 10-20% from baseline. |
| Year 1+ | Continued azoospermia or severe oligospermia in the majority of men not using fertility adjuncts. |
The 2018 Endocrine Society Clinical Practice Guideline explicitly warns that TRT should not be initiated in men actively trying to conceive, and recommends discussing fertility preservation before starting any testosterone therapy [7].
Important: the degree of suppression varies between individuals. Some men retain minimal sperm production on TRT -- enough to occasionally achieve pregnancy -- while others become completely azoospermic within weeks. You cannot predict which category you'll fall into, which is why planning matters.
Strategy 1: HCG Concurrent With TRT
HCG (human chorionic gonadotropin) is the primary tool for preserving fertility while on TRT. It's been the standard of care in fertility-aware TRT clinics for over a decade, and the evidence base is solid.
How It Works
HCG is structurally similar to LH. It binds to the same receptors on Leydig cells and sends the same "produce testosterone" signal. The critical advantage: HCG comes from outside the pituitary, so it works even when your natural LH production is suppressed by exogenous testosterone.
By maintaining stimulation of the Leydig cells, HCG keeps intratesticular testosterone elevated at roughly 25-50% of baseline -- enough to sustain spermatogenesis in most men. A landmark 2005 study demonstrated that even low-dose HCG (250 IU every other day) maintained ITT at 25% of baseline in men whose gonadotropins were completely suppressed by exogenous testosterone [3].
Dosing Protocols
Maintenance protocol (not actively trying to conceive):
- 500 IU subcutaneously, 2-3x per week
- Evenly spaced (Monday/Wednesday/Friday or Monday/Thursday)
- Continue as long as you're on TRT and fertility matters
Active fertility protocol (trying to conceive now):
- 1,000-1,500 IU subcutaneously, every other day
- Combined with FSH if sperm counts remain low after 3 months
- Continue until semen analysis confirms adequate counts
A 2013 study by Coviello et al. confirmed that concomitant intramuscular HCG preserves spermatogenesis in men undergoing TRT, with men maintaining measurable sperm production when HCG was added from the start of testosterone therapy [2].
What to Expect
Most men on concurrent HCG + TRT maintain:
- Measurable sperm counts (though typically lower than pre-TRT baseline)
- 80-90% of baseline testicular volume
- Preserved Leydig cell function for easier future recovery
HCG is not a guarantee of full fertility preservation. Some men still experience significant sperm count reductions even with concurrent HCG. But the difference between "severely reduced" and "zero" is the difference between natural conception being difficult versus impossible.
For a deep dive on HCG protocols, dosing, and monitoring, see our complete HCG fertility guide.
Strategy 2: Enclomiphene Instead of TRT
For men who prioritize fertility above all else, enclomiphene citrate offers a fundamentally different approach: raising testosterone without suppressing the HPG axis.
How It Works
Enclomiphene is the active trans-isomer of clomiphene citrate. It blocks estrogen receptors at the hypothalamus and pituitary, tricking the brain into thinking estrogen is low. The brain responds by increasing GnRH, which raises LH and FSH. Your testes do all the work -- producing both testosterone and sperm through the natural pathway.
Because the HPG axis stays active, spermatogenesis is preserved or even enhanced. A 2015 study showed that enclomiphene raised testosterone levels while simultaneously increasing sperm counts -- something TRT cannot do [6].
Who Should Consider Enclomiphene
Enclomiphene is the better choice when:
- You're under 40 with secondary hypogonadism (the pituitary is the bottleneck, not the testes)
- Fertility is a near-term priority (planning children within 1-5 years)
- Your testosterone deficit is mild to moderate (baseline 200-400 ng/dL)
- You want to avoid the commitment of lifelong TRT
The tradeoff: enclomiphene typically raises testosterone by 200-400 ng/dL over baseline, which is meaningful but less predictable and lower-ceiling than TRT. A man at 250 ng/dL might reach 500-650 ng/dL. If you need 800+ ng/dL for symptom resolution, enclomiphene alone likely won't get you there.
Maximus is one clinic that leads with enclomiphene-first protocols, particularly for younger men where fertility preservation is a priority. For a detailed comparison, see our enclomiphene vs. TRT breakdown.
Strategy 3: FSH Protocols for Recovery
When HCG alone isn't enough -- particularly for men recovering from prolonged TRT without any fertility adjuncts -- adding recombinant FSH can make the difference.
Why FSH Matters
HCG replaces the LH signal but does nothing for FSH. While LH (via HCG) maintains intratesticular testosterone, FSH directly stimulates the Sertoli cells that nurture developing sperm. In men with severely suppressed spermatogenesis, the FSH signal is often the missing piece.
A 2024 study found that combined HCG + FSH therapy recovered spermatogenesis in 74% of men with testosterone-induced infertility. The average time to recovery was 4.6 months, with a mean first sperm density of 22.6 million/mL [5].
Typical FSH Protocol
- Medication: Recombinant FSH (follitropin alfa or beta)
- Dose: 75 IU subcutaneously, 3x per week
- Combined with: HCG 1,000-3,000 IU every other day
- Duration: 3-6 months minimum, guided by semen analysis
- Monitoring: Semen analysis every 6-8 weeks; FSH, LH, and testosterone labs monthly
FSH is significantly more expensive than HCG -- typically $200-500 per month depending on the formulation. But for men who've been azoospermic on TRT for years and need to recover fertility, the combination protocol has the highest success rate documented in the literature.
When to Escalate to FSH
Consider adding FSH to HCG if:
- HCG monotherapy for 3+ months hasn't improved semen analysis
- You've been on TRT for >2 years without any fertility preservation
- You need to conceive within a specific timeframe and can't afford to wait